top of page
After hours: If urgent, life threatening (please call 988, 911, or go to nearest ER. Otherwise, for side effects to medications, please text 816-766-0119. For all other non-urgent issues, please contact us Practice Q messaging portal or contact us during clinic hours at 888-855-0947.

Mental health providers

a women crying while holding a hand

a boy bow down on floor

Mental health providers
1/3
Ready for your Mental Health Transformation?
Child Psychiatrist /Adult Psychiatrist

Blog
Search


How Ketamine Therapy Is Changing Depression Treatment
Depression is one of the most common mental health disorders globally, affecting millions of people each year. While traditional therapies like antidepressants and psychotherapy have benefited many people, a large number of patients continue to suffer from symptoms despite trying various therapies. This illness is commonly referred to as treatment resistant depression. Ketamine therapy has recently emerged as a game changing potential in mental health treatment. Developed ini

Vilash Reddy, MD
May 273 min read


How Magic Mushrooms May Treat Mental Illness
In recent years, magic mushrooms, a colloquial phrase for fungi containing the hallucinogenic chemical psilocybin, have progressed from a counterculture curiosity to a significant psychiatric study topic. Scientists and physicians are now looking into whether psilocybin assisted therapy could be a new paradigm for treating mental illnesses, particularly those that are resistant to traditional therapies. What are Magic Mushrooms? Magic mushrooms contain psilocybin, a naturally

Vilash Reddy, MD
May 13 min read


Support for Families Dealing with Bipolar Disorder
Supporting a loved one with bipolar disorder can be emotionally hard, difficult, and often overwhelming. Families frequently find themselves managing unpredictable mood swings, ranging from manic highs to depressive lows, while attempting to preserve everyday stability. Understanding the disease and understanding how to respond successfully are critical not just for the individual diagnosed, but also for the overall well-being of the family system. Bipolar disorder is a chron

Vilash Reddy, MD
Apr 203 min read


Rare Sexual Disorders in Men May Challenge Diagnosis
Erectile dysfunction, premature ejaculation, and hypogonadism are common clinical diagnoses. Beyond established guidelines, however, there is a group of rare sexual disorders in men that are often overlooked or prematurely classified as psychogenic disorders. For affected individuals, this can lead to prolonged evaluation across multiple specialties and substantial impairment of their quality of life, intimate relationships, and mental health. A review published in Nature Rev

Vilash Reddy, MD
Apr 35 min read


The Financial Costs of Schizophrenia
The direct and indirect costs of schizophrenia cause a sizable societal burden. Key points Schizophrenia is a chronic disorder affecting over 1 percent of the U.S. population. The annual societal costs per affected individual range from about $111,000 to $126,000 annually. Twenty percent of these costs result from direct expenses like health care, housing, and disability benefits. Costs can be lowered by investing in research that will lead to prevention and better treatments

Vilash Reddy, MD
Mar 313 min read


Is Social Media Addiction Real?
Two years ago, US Surgeon General Vivek Murthy, MD, called for warning labels on social media platforms, citing concerns about the potential mental health risks associated with heavy use, especially among children, adolescents, and young adults. The debate has intensified as researchers investigate how heavy social media use affects brain development, mood, and cognition and whether patterns of heavy social media use resemble behavioral addictions. That scrutiny reached a tur

Vilash Reddy, MD
Mar 276 min read


A Potential New Treatment for PTSD
A drug that stimulates neuronal growth decreases PTSD symptoms. Key points Current treatments for PTSD have limited effectiveness. Some research suggests that MDMA (Ecstasy) together with psychotherapy may reduce PTSD symptoms. Methylone is produced by modifying the chemical structure of MDMA. Methylone, without psychotherapy, led to clinically meaningful improvement of PTSD symptoms. by Eugene Rubin MD, PhD and Charles Zorumski MD Posttraumatic stress disorder (PTSD) is a di

Vilash Reddy, MD
Mar 215 min read


Does Cannabis Really Help PTSD? New Data Cast Doubt
New research challenges the assumption that long-term cannabis use improves symptoms or functioning in post-traumatic stress disorder (PTSD). On the contrary, researchers found that abstaining from cannabis for 3 months was associated with significantly greater reductions in PTSD symptoms in adults with PTSD and comorbid cannabis use disorder (CUD). The data suggest that continued cannabis use could limit recovery in some domains — underscoring the need to routinely assess ca

Vilash Reddy, MD
Mar 193 min read


Social Media Use Linked to Depression, Lower Grades in Children
TOPLINE: Digital media use in children and adolescents was associated with poorer developmental outcomes, with social media showing the most consistent adverse links to depression, behavioral problems, and substance use. Video gaming was linked to aggression and externalizing behaviors. METHODOLOGY: Researchers conducted a systematic review and meta-analysis of longitudinal studies examining the associations between the use of digital media and health and developmental outcom

Vilash Reddy, MD
Mar 172 min read


Cutting Through the Noise on Neurodivergence in Medicine
Neurodiversity is often in the headlines, with articles ranging from scaremongering about an explosion in diagnoses to helpful and informative pieces on how best to support neurodivergent family, friends, and colleagues. The amount of information available can feel overwhelming and confusing, given the proliferation of opinion on the issue. As a neurodivergent individual myself, navigating this range of content can be challenging and frustrating. One moment it feels supportiv

Vilash Reddy, MD
Mar 174 min read


New Deprescribing Guidance Marks an ‘Important Moment’ in Psychiatry
A new expert consensus statement from the American Society of Clinical Psychopharmacology offered clinical guidance on when and whether to discontinue psychiatric medications. The statement, developed by a 45-member international task force, reached consensus on 44 of 50 recommendations addressing when deprescribing is warranted. Among the key points: clinicians should periodically reassess all medications, always verify adherence before concluding a drug isn’t working, and e

Vilash Reddy, MD
Feb 265 min read


Why Pediatricians Need Training in Psychiatry
Key points Pediatricians have experienced a dramatic increase in patient visits for psychiatric conditions. This increase has occurred in both children (age 4 to 12) and adolescents (age 13 to 17). Much of this increase is attributed to an increase in anxiety disorders. It is critical that pediatric residents receive adequate exposure to child and adolescent psychiatry. Much has been written recently about an increase in the number of American youths experiencing mental healt

Vilash Reddy, MD
Feb 203 min read


Trauma Survivor or Trauma Victim What’s the Right Term?
After experiencing severe trauma and neglect, the path from victim to survivor or conversely, staying in a cycle of suffering is driven by a complex interplay of internal coping mechanisms and external support systems. Factors for Becoming a Survivor: Transitioning to a survivor requires establishing physical safety, receiving social support, and reclaiming one's life story, allowing the individual to integrate the trauma rather than being ruled by it. Survivors often develo

Vilash Reddy, MD
Feb 114 min read


Are PTSD and Autism Separate Conditions?
Complex Post-Traumatic Stress Disorder (CPTSD) and Autism Spectrum Disorder (ASD) often overlap in observable behavior, particularly in social settings, though their internal motivations differ significantly. Individuals with extensive CPTSD may identify with autism to normalize their difficulties connecting with others, as it frames these challenges as a fundamental difference in "wiring" rather than just a response to injury. Reasons for Identification Symptom Overlap: Bot

Vilash Reddy, MD
Feb 112 min read


Savant or Gifted? How ADHD and Autism Change the Picture
ADHD (Attention-Deficit/Hyperactivity Disorder) and Autism Spectrum Disorder (ASD) frequently co-occur (often referred to as AuDHD), with 50-70% of autistic people also having ADHD. While they are distinct neurodevelopmental conditions, they share significant overlaps in traits and often appear together, creating unique strengths and challenges. Advantages of Having ADHD and/or Autism (AuDHD) When occurring together (AuDHD), the combination can create a unique balance between

Vilash Reddy, MD
Feb 93 min read


How ADHD Differs From Autism Spectrum Disorder
In evolutionary terms, neurodivergence is often viewed not as a collection of "errors," but as adaptive variations that ensured the survival of early human groups through cognitive specialization. Evolutionary Origins and Roles Evolutionary theories suggest these conditions persist because they offered specific benefits to the collective "cognitive ecology" of a tribe or clan. ADHD (The "Hunter" Role): Traits like hyperactivity and rapid attentional shifts were advantageous

Vilash Reddy, MD
Feb 93 min read

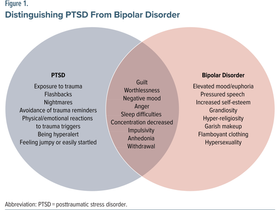
Mood Swings or Trauma Responses? Bipolar vs CPTSD
In 2026, the misdiagnosis of Complex Post-Traumatic Stress Disorder (CPTSD) and Borderline Personality Disorder (BPD) as Bipolar Disorder remains a significant issue in adult psychiatry. This frequently occurs due to overlapping symptoms, institutional barriers, and a lack of trauma-informed training among medical professionals. Why Misdiagnosis Occurs Symptom Overlap: Symptoms of hyperarousal in CPTSD—such as irritability, racing thoughts, and insomnia—closely mimic the hy

Vilash Reddy, MD
Feb 62 min read


Types of Dissociative Identity Disorder (DID)
Dissociative Identity Disorder (DID) typically develops as an extreme survival mechanism in early childhood . In the case described, the "bold guardian" and "weak depressed" parts likely formed due to severe developmental pressure in a high-stakes, punitive environment. Why DID Developed This Way The "Guardian" Part: Often called Protectors or Caretakers, these identities emerge to handle situations the child (the "host") cannot endure. In a hyper-religious, punitive househo

Vilash Reddy, MD
Feb 63 min read


Is Telepsychiatry Good or Bad?
The Ryan Haight Online Pharmacy Consumer Protection Act of 2008 was enacted to close a specific legal loophole that allowed "rogue" online pharmacies to dispense controlled substances without a physical medical exam. While the broader opioid epidemic involved complex issues with manufacturers like Purdue Pharma and in-person medical practices, the Ryan Haight Act targeted a new, unregulated frontier: the internet. Why Ryan Haight Was "Special" Ryan Haight was an 18-year-old h

Vilash Reddy, MD
Feb 62 min read


Why do Patients Hate Psychiatrists?
While exact global counts of psychiatrists specializing in psychodynamic psychotherapy for 2026 are not available, specific trends highlight a growing shortage of these specialists despite their high efficacy in treating complex mental disorders. Specialist Availability and Efficacy Provider Landscape: Approximately 25% of psychotherapists currently utilize psychodynamic methods. Workforce Trends: As of 2026, the United States faces a significant shortage, with the total ps

Vilash Reddy, MD
Feb 33 min read
bottom of page

