top of page
After hours: If urgent, life threatening (please call 988, 911, or go to nearest ER. Otherwise, for side effects to medications, please text 816-766-0119. For all other non-urgent issues, please contact us Practice Q messaging portal or contact us during clinic hours at 888-855-0947.

Mental health providers

a women crying while holding a hand

a boy bow down on floor

Mental health providers
1/3
Ready for your Mental Health Transformation?
Child Psychiatrist /Adult Psychiatrist

Blog
Search


New Deprescribing Guidance Marks an ‘Important Moment’ in Psychiatry
A new expert consensus statement from the American Society of Clinical Psychopharmacology offered clinical guidance on when and whether to discontinue psychiatric medications. The statement, developed by a 45-member international task force, reached consensus on 44 of 50 recommendations addressing when deprescribing is warranted. Among the key points: clinicians should periodically reassess all medications, always verify adherence before concluding a drug isn’t working, and e
Vilash Reddy, MD
Feb 265 min read


Why Pediatricians Need Training in Psychiatry
Key points Pediatricians have experienced a dramatic increase in patient visits for psychiatric conditions. This increase has occurred in both children (age 4 to 12) and adolescents (age 13 to 17). Much of this increase is attributed to an increase in anxiety disorders. It is critical that pediatric residents receive adequate exposure to child and adolescent psychiatry. Much has been written recently about an increase in the number of American youths experiencing mental healt
Vilash Reddy, MD
Feb 203 min read


Trauma Survivor or Trauma Victim What’s the Right Term?
After experiencing severe trauma and neglect, the path from victim to survivor or conversely, staying in a cycle of suffering is driven by a complex interplay of internal coping mechanisms and external support systems. Factors for Becoming a Survivor: Transitioning to a survivor requires establishing physical safety, receiving social support, and reclaiming one's life story, allowing the individual to integrate the trauma rather than being ruled by it. Survivors often develo
Vilash Reddy, MD
Feb 114 min read


Are PTSD and Autism Separate Conditions?
Complex Post-Traumatic Stress Disorder (CPTSD) and Autism Spectrum Disorder (ASD) often overlap in observable behavior, particularly in social settings, though their internal motivations differ significantly. Individuals with extensive CPTSD may identify with autism to normalize their difficulties connecting with others, as it frames these challenges as a fundamental difference in "wiring" rather than just a response to injury. Reasons for Identification Symptom Overlap: Bot
Vilash Reddy, MD
Feb 112 min read


Savant or Gifted? How ADHD and Autism Change the Picture
ADHD (Attention-Deficit/Hyperactivity Disorder) and Autism Spectrum Disorder (ASD) frequently co-occur (often referred to as AuDHD), with 50-70% of autistic people also having ADHD. While they are distinct neurodevelopmental conditions, they share significant overlaps in traits and often appear together, creating unique strengths and challenges. Advantages of Having ADHD and/or Autism (AuDHD) When occurring together (AuDHD), the combination can create a unique balance between
Vilash Reddy, MD
Feb 93 min read


How ADHD Differs From Autism Spectrum Disorder
In evolutionary terms, neurodivergence is often viewed not as a collection of "errors," but as adaptive variations that ensured the survival of early human groups through cognitive specialization. Evolutionary Origins and Roles Evolutionary theories suggest these conditions persist because they offered specific benefits to the collective "cognitive ecology" of a tribe or clan. ADHD (The "Hunter" Role): Traits like hyperactivity and rapid attentional shifts were advantageous
Vilash Reddy, MD
Feb 93 min read

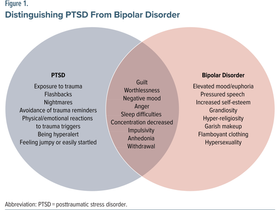
Mood Swings or Trauma Responses? Bipolar vs CPTSD
In 2026, the misdiagnosis of Complex Post-Traumatic Stress Disorder (CPTSD) and Borderline Personality Disorder (BPD) as Bipolar Disorder remains a significant issue in adult psychiatry. This frequently occurs due to overlapping symptoms, institutional barriers, and a lack of trauma-informed training among medical professionals. Why Misdiagnosis Occurs Symptom Overlap: Symptoms of hyperarousal in CPTSD—such as irritability, racing thoughts, and insomnia—closely mimic the hy
Vilash Reddy, MD
Feb 62 min read


Types of Dissociative Identity Disorder (DID)
Dissociative Identity Disorder (DID) typically develops as an extreme survival mechanism in early childhood . In the case described, the "bold guardian" and "weak depressed" parts likely formed due to severe developmental pressure in a high-stakes, punitive environment. Why DID Developed This Way The "Guardian" Part: Often called Protectors or Caretakers, these identities emerge to handle situations the child (the "host") cannot endure. In a hyper-religious, punitive househo
Vilash Reddy, MD
Feb 63 min read


Is Telepsychiatry Good or Bad?
The Ryan Haight Online Pharmacy Consumer Protection Act of 2008 was enacted to close a specific legal loophole that allowed "rogue" online pharmacies to dispense controlled substances without a physical medical exam. While the broader opioid epidemic involved complex issues with manufacturers like Purdue Pharma and in-person medical practices, the Ryan Haight Act targeted a new, unregulated frontier: the internet. Why Ryan Haight Was "Special" Ryan Haight was an 18-year-old h
Vilash Reddy, MD
Feb 62 min read
bottom of page

